What is Chronic Venous Disease (CVD)?
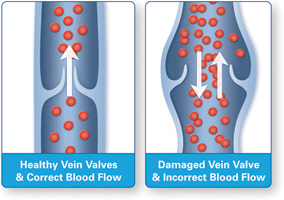
Your veins are part of a low-pressure drainage system which takes the used blood back to your heart. A healthy vein contains valves which open and close to keep the blood moving in the right direction. Problems develop when some of those valves become damaged and stop working. This results in backward flow (“reflux”) of blood in the veins, and a slower drainage of the used blood from your legs. This is called Chronic Venous Disease (CVD).
What should I look for?
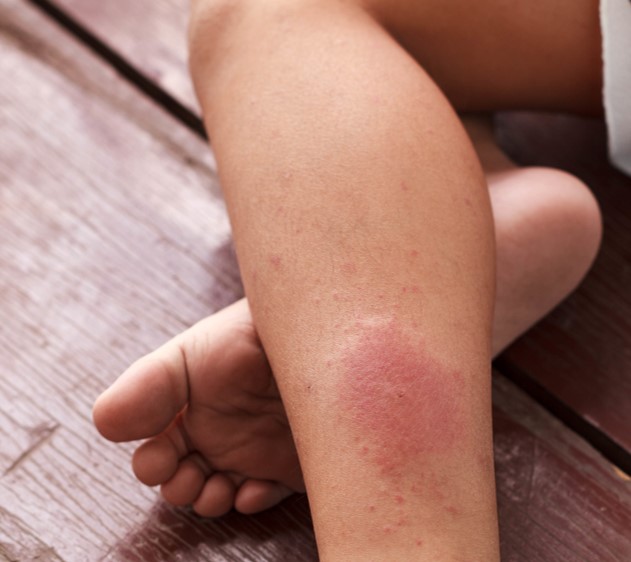
Common signs and symptoms of CVD in the legs include pain, discomfort, fatigue, prominent veins, swelling, and in advanced cases, skin changes, and ulcerations.
- Leg pain
- Leg discomfort (itching/cramping/restless legs/heaviness)
- Leg fatigue
- Spider Veins
- Varicose Veins
- Swelling/ “Edema”
- Skin changes/ “Stasis Dermatitis”
- Ulceration
Who is at risk?
Some risk factors for CVD are out of your control. These include family history, sex, and age. Other risk factors can be controlled. These include obesity, pregnancy, having a job that requires prolonged sitting or standing, injury, surgery, and blood clots.
- Family History
- Sex (Females have more risk)
- Age (Risk increases with age)
- Obesity
- Pregnancy
- Prolonged standing or sitting
- Prior injury or surgery
- History of blood clot
How common is CVD?
If you suffer from problems related to CVD, you are not alone. More than 30 million Americans suffer from CVD, but only about 1.9 million people (6%) seek treatment each year. The main reason this number is so low is the fact that most people are not aware that CVD is more than just a cosmetic issue, and that it is treatable.
How is CVD treated?
In the past, CVE was treated with vein stripping, a painful, invasive surgical procedure. Thankfully, there are better options now. The first step in management is usually a trial of conservative measures. We perform minimally-invasive procedures in the comfort of our office. We use local much less post-operative pain and recovery times. Patients are often surprised to learn that since CVD is an accepted medical condition, most of our procedures are covered by medical insurance.